HIATAL HERNIA
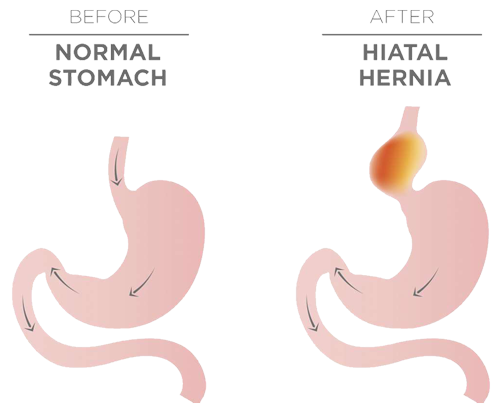
Any time an internal body part pushes into an area where it doesn’t belong, it’s called a hernia. The hiatus is an opening in the diaphragm – the muscular wall separating the chest cavity from the abdomen. Normally, the esophagus goes through the hiatus and attaches to the stomach. In a hiatal hernia, the stomach bulges up into the chest through that opening. Para-esophageal hernias are less common large hiatal hernias. When they start to cause symptoms (chest pain, upper abdominal pain, difficulty swallowing), it is a cause for concern and these should be repaired. Symptomatic para-esophageal hernias are at higher risk for progressing to incarceration (stomach gets stuck resulting in obstruction) or ischemia (blood supply to the stomach is cut off) resulting in the need for emergency surgery.
SYMPTOMS:
- Heartburn
- Sudden chest pain
- Difficulty swallowing
- Shortness of breath
- Stomach pain
- Indigestion
- Nausea and vomiting
DIAGNOSING HIATAL HERNIAS:
Upper gastrointestinal series
This is a series of X-rays in which you drink a white, chalky liquid (barium) that coats the digestive system to help abnormalities show up. This is very helpful in determining the size of a hiatal hernia.
48 hour Ambulatory acid (pH) probe test
A small probe is placed in your esophagus to identify when, and for how long, stomach acid regurgitates there. The monitor connects to a small computer that you wear around your waist or with a strap over your shoulder. The probe is placed in your esophagus during an endoscopy. The test lasts two days. The probe then falls off of the esophagus and is passed into your stool after about one week.
Upper gastrointestinal (GI) endoscopy
This procedure is used to visually examine your upper digestive system — your esophagus, stomach and beginning of the small intestine (duodenum) — with a tiny camera on the end of a long, flexible tube (Video-endoscopy). This test can also diagnose other conditions, such as peptic ulcer disease or pyloric stenosis, which can have symptoms similar to those of a hiatal hernia.
Esophageal manometry
This test measures the rhythmic muscle contractions in your esophagus when you swallow. A small tube is placed into the esophagus and attached to a monitor. You are then asked to swallow a small amount of water 10 times and the pressures within the esophagus are checked. Esophageal manometry also measures the coordination and force exerted by the muscles of your esophagus.
TREATMENT:
The use of advanced laparoscopic techniques in the management of patients with large type II, type III, and type IV para-esophageal hernias has completely changed the treatment of this condition. Typically, patients with these types of hernia are older and have multiple medical conditions. In the past, many patients were not referred for surgery because of concerns that they would not survive this type of surgery which was performed through large chest incisions. Patients would be in the hospital for weeks with high rates of complications.
Para-esophageal hernias are now repaired using an abdominal approach with advanced laparoscopic techniques. Patients experience minimal pain with the surgery and are usually home in 1-2 days – even older patients. More importantly, the use of new types of mesh to reinforce the hiatal hernia repairs has markedly decreased the recurrence rates. Patients now can expect to have a big operation through small incisions that leaves them with an excellent quality of life.